A TORTURED PATH: Curare’s Journey from Poison Darts to Paralysis by Design
Frederick Prescott called the experience terrifying (1). Scott Smith still vividly recalled, thirty years later, feeling a level of anxiety and panic that bordered on psychosis (2, 3). Unable to move or breathe, both men remained fully conscious and their senses were, if anything, more acute.
In the 1940s, curare, a new drug in the anesthesiologist’s toolbox, was rapidly gaining popularity, but it was also raising concerns. The drug’s paralytic actions had been consistently reproduced in laboratory experiments for decades; however, other putative effects on the heart and central nervous system were derived from observations that were both confusing and contradictory. Some thought the drug caused unconsciousness, others did not. To settle the growing controversy, Prescott and Smith in separate studies on different continents volunteered to serve as their own test subjects. When they recovered from the drug’s effects, their graphic first-person accounts left no doubts. Curare was definitely not an anesthetic or an analgesic.
Early History of Curare
The discovery of curare is veiled in the unrecorded history of native South American tribes, who smeared the substance on their blow darts and arrowheads to improve their chances of bagging wild game. The first published account, which described Sir Walter Raleigh’s 1595 voyage up the Amazon, gave dramatic eye-witness descriptions of expedition colleagues succumbing to the effects of poison arrows (4, 5). In the centuries that followed, exaggerated tales emerged about this mythical poison, and the Europeans mistakenly concluded that its efficacy was somehow related to the type of vessel in which it was stored: finger-sized bamboo tubes; small earthen pots; or dried, hollow gourds. They classified the poison as tube, pot, and calabash curare, respectively (4–6).
“Potency was titrated by bioassay as either “one-tree” curare if a wounded monkey could make only one leap before collapsing or “three-tree” curare if the animal could be captured alive.”
Between 1799 and 1804, Alexander von Humboldt trekked ancient Inca trails and surveyed the headwaters of the Amazon. Later, he published the first recipe for the Indian’s poison, a tar-like mass that the natives called curari, woorari, or wourali (4, 6, 7). Potency was titrated by bioassay as either “one-tree” curare if a wounded monkey could make only one leap before collapsing or “three-tree” curare if the animal could be captured alive (4).
Nineteenth century scientists furthered their understanding of curare’s properties through insightful observations and methodically conducted laboratory experiments. In 1812, Charles Waterton explored Guiana and Brazil and described how an ass was revived by artificial respiration after it had presumably died from a wourali-poisoned wound. Claude Bernard, in a series of experiments, showed that intravenous injection of the arrow poison paralyzed the chest and abdominal muscles of frogs and caused death by respiratory failure. In 1844, he used frog nerve-muscle preparations to show that curare blocked cholinergic neuromuscular transmission (4, 5, 7). Impressed by Bernard’s observations, clinicians in France and Germany explored using curare to relax the muscles of tetanus, epilepsy, and chorea patients. By the end of the nineteenth century, however, these efforts were abandoned because curare was considered too dangerous to use therapeutically (5, 7).
Curare’s therapeutic utility resurfaced in the 1930s, but progress was handicapped by a lack of knowledge about curare’s composition and source (5, 7). Native shamen tenaciously guarded their secrets and were unwilling to share the plant sources and curare preparation with outsiders (8). Without access to fresh material, Harold King, at the National Institute for Medical Research in London, secured an old, dried specimen of tube curare from the Ceramics Department of the British Museum. In 1935, King isolated a potent alkaloid from the crude plant extract (4, 5, 9), thus, calling the isolated alkaloid d-tubocurarine (4).
Richard Gill’s Quest
Curare became a useful research tool for physiologists who understood its effect on neuromuscular transmission. But the compound might never have advanced beyond a laboratory curiosity if not for the tenacious and patiently persistent efforts of Richard Gill (8).
Born in Washington, D.C., in 1901, Gill studied at Cornell University. He was expected to follow his father and older brother into the practice of medicine; however, he grew restless and interrupted his studies to join a whaling fleet in Alaska. He subsequently traveled widely, taking a series of odd jobs, and finally after earning a degree in English at Cornell, he served as an agent for the American Rubber Company in Peru. Losing that job after the 1929 stock market crash, Gill bought a plantation near Banos, Ecuador, built a hacienda, and began raising tropical fruits (8).
While on a visit to the United States in 1932, Gill was thrown from his horse and developed a neurological syndrome that worsened over the next two years until he was completely incapacitated. Suffering painful muscle spasms that did not respond to conventional treatment, Gill was encouraged when his neurologist suggested that the South American arrow poison might alleviate his spasticity; unfortunately, clinical samples were not available. The hope of a treatment spurred Gill’s determination to conquer his illness and return to South America. He underwent years of intensive physiotherapy while simultaneously teaching himself medicine, pharmacology, botany, and related subjects (8, 10, 11).
In 1938, again able to walk, Gill led a four month expedition to Ecuador, lugging tons of equipment and supplies into the dense rain forests. For years at his hacienda, he had patiently studied the customs of the indigenous people, respected their culture and beliefs, and gradually earned their trust. Now, he nurtured that relationship further, and his patient but persistent efforts were rewarded (8, 10).
The natives elevated Gill to the status of a shaman and divulged their secret ingredients and recipes for the arrow poison (8). In an intricate, days-long ceremony filled with rituals, they boiled down and strained the roots, bark, and stems of a large, tropical vine, Chondrodendron tomentosum, allowing the resulting liquid to thicken into a gummy paste.
The paste was then stored for future use in the tube, pot, or gourd containers (6).
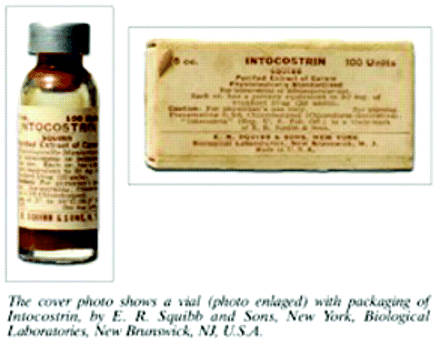
Gill returned to the United States with twenty-five pounds of crude curare paste and more than seventy species of medicinal jungle plants, including C. tomentosum (8, 10). He gave curare samples to a number of clinicians and shopped the drug to several pharmaceutical companies, mostly without success. After the popular memoir of his experiences, White Water and Black Magic, was published in 1940, he managed to attract the interest of researchers at E. R. Squibb & Sons (4, 6, 8).
Pharmaceutical Interest in Curare
Gill gave the bulk of his crude curare to Squibb, and after internal testing the company marketed a sterile but impure form of curare called Intocostrin® (6, 10). Vials of 5 and 10 ml contained 20 mg of “curare extract” per ml, and the recommended adult dose was 50 to 60 mg, given intravenously (9).
In 1936, Burroughs Wellcome had begun research with curare at its Chemical Works in Dartford and Physiological Research Laboratories in Beckenham, UK (7). Exploiting King’s purification method and Gill’s identification of C. tomentosum as the source, the researchers isolated several alkaloids with muscle relaxant properties from crude curare (e.g., curine, protocurine, and chondrodendrine). Nevertheless, d-tubocurarine was the most selective muscle relaxant compound, and the company marketed the crystalline alkaloid as Tubarine® (5, 7). Ampoules of 1.5 and 5 ml contained a concentration of 10 mg of d-tubocurarine chloride per ml, and the recommended adult dose was 25 to 30 mg, given intravenously (7, 9).
Both companies calibrated the potency of their products by bioassay, finding the rabbit head-drop test more convenient than watching monkeys fall out of trees (5, 10). Despite marketing campaigns, clinical acceptance, especially as an anesthesia adjunct, was slow in coming. Curare was, after all, a potent poison and could kill if used incorrectly.
Testing Curare in Humans
In the 1930s, anesthesiologists’ choices for general anesthesia were limited to nitrous oxide, cyclopropane, ether, and thiopental, all of which had weak muscle relaxant properties (5). To achieve the muscle relaxation desired for abdominal and thoracic surgery, they needed to induce deep general anesthesia, which not only necessitated controlled, artificial ventilation but also prompted other secondary complications including shock, hypotension, and vomiting (5, 7, 8).
A better, more selective muscle relaxant, such as curare, would overcome these problems. Nevertheless, Squibb had to vigorously promote its product (8, 10). After failing to interest several prominent anesthesiologists, Squibb’s medical director recommended the drug to Harold Griffith, a part-time anesthesiologist at the Homeopathic Hospital in Montreal. Griffith and his resident, Enid Johnson, administered Intocostrin during appendectomies and intraperitoneal operations (7, 8, 10). Their 1942 publication, reporting that the abdomen was “as soft as dough” after curare administration, became the pivotal event leading to the drug’s expanded use during surgery (8, 10, 12).
As an adjunct to anesthesia, curare was soon hailed as the greatest advance since the discovery of intravenous anesthesia (5). In 1945, the American Medical Association’s Council on Pharmacy and Chemistry accepted Intocostrin for inclusion in New and Nonofficial Remedies (2). In 1946, Gray and Halton were the first to report using Burroughs Wellcome’s d-tubocurarine as an adjunct to anesthesia (1).
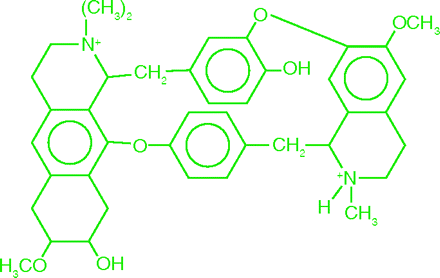
Today, any pharmacology student who looks at the structure of d-tubocurarine, with its two quaternary nitrogens, rapidly concludes that the molecule cannot cross the blood-brain barrier and, therefore, has no central anesthetic effects. The polar molecular structure also explains how the South American natives could eat their curare-tainted prey without ill effects. But in the 1940s, the pharmacology of curare, aside from its well-established action as a neuromuscular blocker, was not so clear.
A number of studies in various animal species reported an apparent depressant effect of curare on the central respiratory center, auditory cortex, and brain electrical activity. Other animal studies suggested that curare had an excitatory effect on the brain and spinal cord. Claims of analgesic effects, both in humans and animals, were also reported but were confounded by poorly controlled experimental conditions and the subjectivity of pain perception (2).
Although the drug’s central actions on consciousness and pain perception were far from established, some anesthesiologists were beginning to use curare during surgery in conjunction with only pre-anesthetic medication (such as atropine and local anesthetics). In a few surgical cases, primarily in infants and children, curare had been given without any type of anesthetic (2, 13).
To settle the question of curare’s putative anesthetic and analgesic effects, Frederick Prescott and Scott Smith decided to subject themselves to the drug under clinically controlled conditions. In those days, before oversight by regulatory authorities and institutional review boards, self-experimentation was a rather common practice. Their medical ethics dictated that the investigator should not expose other humans to an experimental agent unless he first experienced the consequences himself.
Frederick Prescott and Burroughs Wellcome
Born in 1904 in London, Frederick Prescott earned master’s and PhD degrees from University College, London. He then taught and authored several chemistry textbooks before turning to medicine. In 1938, he received his medical credentials from Middlesex Hospital Medical School and joined Roche Products Ltd. as Medical Director, where he investigated the uses of new drugs. In 1941, Prescott became Director of Clinical Research at the Wellcome Research Institute, where he was responsible for the medical research of Burroughs Wellcome products. Because Squibb’s product was a crude curare extract and Burroughs Wellcome was preparing to market the purified alkaloid of curare, Prescott and his colleagues were concerned about differences in potency of the two products. Wellcome’s Tubarine appeared to be three times more potent than the Squibb extract and might cause serious overdosing if misused (1).
Starting sometime in 1945, the scientists at Burroughs Wellcome conducted a clinical study to establish their product’s optimal dose level, dose schedule, and route of administration. Prescott, who was forty-one and the research institute’s clinical director, was the obvious first test subject. Anesthetist Sir Geoffrey Organe and the anesthesia staff at Westminster Hospital provided supportive care (1). They agreed on a set of hand signals so that Prescott could inform his colleagues if he became too weak or had difficulty breathing.
Intravenous doses of 10 and 20 mg of d-tubocurarine produced mild to moderate weakening of his facial, laryngeal, limb, abdominal, and intercostal muscles and a slight reduction in respiratory tidal air volume. At each dose, the onset and duration of the drug’s effects were short, and Prescott completely recovered in three to four hours (1).
Emboldened by these initial results, Prescott was then given a 30 mg dose intravenously. Within minutes, he experienced complete skeletal muscle paralysis. His colleagues, who were chatting lightheartedly at his bedside, were initially unaware of his asphyxia, which he tactfully described in his published report as “a very unpleasant experience” (1). After five agonizing minutes, unable to use his hand signals, and just as he was losing consciousness from poor oxygen exchange and accumulating airway mucus, Prescott’s colleagues finally noticed his difficulty. They administered artificial respiration for seven minutes, after which he had recovered sufficiently to breathe on his own. Continuing with the experimental protocol, they tore adhesive strips from a hairy patch of Prescott’s skin, a procedure that he said produced considerable pain (1). Most of the drug’s effects reversed after four to six hours, but Prescott experienced lingering thoracic tightness for several days.
Prescott and his colleagues continued their investigations on him by next exploring various bolus and continuous infusion dosing schemes and the pharmacokinetics of intravenous versus intramuscular administration. Assay of his urine confirmed that at least some of the drug was excreted unchanged. Armed with these data, the Burroughs Wellcome group proceeded with a clinical study administering d-tubocurarine, in conjunction with standard general anesthetics, to 180 patients who were undergoing various surgical procedures. The results of these investigations, published in July 1946, represented the first comprehensive report of d-tubocurarine’s clinical pharmacology (1) and formed the basis of the company’s dosing instructions to physicians (7).
Scott Smith and the University of Utah
Born in Missouri in 1912, Scott Smith received his bachelor’s degree from the University of Missouri and, in 1939, his medical degree from the University of Louisville. After severe radiation burns from a defective fluoroscope during his residency training ended his ambitions of becoming a surgeon, Smith turned to the emerging field of anesthesiology. After completing his anesthesiology residency at the University of Minnesota in 1943, he headed to California to pursue an anesthesiologist position. During the train’s stop-over in Salt Lake City, Utah, Smith learned that the University of Utah’s new four-year medical school was seeking a faculty member in anesthesiology (3).
Smith accepted the position of instructor of anesthesiology, thinking that he could steer his career toward teaching if his injured hand limited his ability to practice. In addition to his part-time faculty appointment, Smith provided anesthesia services at LDS Hospital and Salt Lake General Hospital. In 1945, Smith, who was now a part-time assistant clinical professor, was named head of the University of Utah’s newly created anesthesiology department. He launched an anesthesiology residency training program and also trained nurse anesthetists (3).
Six months before Prescott’s paper was published, Smith became increasingly concerned about the conflicting accounts of curare’s putative central actions and decided to conduct his own experiment. He obtained a sample of d-tubocurarine from Squibb and was assisted in his study by several Utah faculty colleagues including pharmacology chairman Louis Goodman (2). At Burroughs Wellcome, Prescott had undergone a series of exposures to curare. For Smith, once was enough.
On January 10, 1946, Smith, who was thirty-three, began a long afternoon of curare infusions and clinical assessments. The investigators had agreed on a hierarchy of communications, starting with verbal responses until Smith could no longer speak, signaling via voluntary contraction of nonparalyzed muscles until he could no longer move, and ultimately making mental notes, which Smith dictated to a stenographer immediately after recovery (2).
“At Burroughs Wellcome, Prescott had undergone a series of exposures to curare. For Smith, once was enough.”
Over thirty-five minutes, Smith received incremental intravenous curare doses that totaled 2.5-times the dose necessary to produce complete paralysis. Artificial respiration with oxygen was administered during the hour-long interval when Smith was unable to breathe on his own. For eleven excruciating minutes, he was unable to move any skeletal muscle or communicate his distress. Despite periodic aspiration of accumulating secretions, Smith experienced sensations of shortness of breath and choking similar to drowning. When he was finally able to give a weak voluntary signal (by wrinkling his forehead), he responded to his colleagues’ questions, vigorously wrinkling to indicate that he wanted more frequent aspiration (2).
Various tests of memory, decision making, and sensory perception were administered throughout the experiment. Heat, cold, and jabs by pinprick were all perceived normally. Smith distinguished colors and could distinctly hear conversations, even when his colleagues were whispering at a distance. He accurately remembered the proper temporal sequence of events that occurred throughout the experiment, including several details that his colleagues had either forgotten or failed to record (2).
Four hours after the initial infusion, Smith had recovered most motor function, but some skeletal muscle weakness persisted throughout the evening. The investigators published their experiment as a case study in January 1947 (2).
Recommendations and Reactions
Despite differences in experimental design, Prescott and Smith reported strikingly similar experiences. First and foremost, curare had no effect on sensory perception, mental acuity, or consciousness. Second, skeletal muscle paralysis changed respiratory dynamics such that both men felt under-ventilated, even when their colleagues were applying artificial respiration within the “normal” range. Smith later said he “would have given anything to be able to take one deep breath” (2). Finally, although both men exhibited elevated blood pressure and heart rate, neither attributed this to an effect of curare on the cardiovascular system. As Prescott explained in characteristic British understatement, “the effect of emotion cannot be excluded: indeed one cannot be paralyzed and remain perfectly tranquil” (5).
The two clinicians also came to identical conclusions and made the same recommendations about curare’s use in anesthesia. Both acknowledged that curare’s muscle relaxant actions were especially useful to surgeons performing thoracic and abdominal operations; however, they emphasized that the drug should only be used in combination with general anesthetics and appropriate analgesics (1, 2). Curare should never be used as the sole agent in an otherwise conscious patient because “the effects are far too unpleasant” (1).
When their respective reports were published, it created a brief sensation in the lay press, which sported headlines like, “Doctor Died for Seven Minutes” (4). The public attention helped ensure a speedy entry of curare into clinical use. It also ignited a search for new and better agents because, as a plant extract, d-tubocurarine supplies were limited and expensive (1).
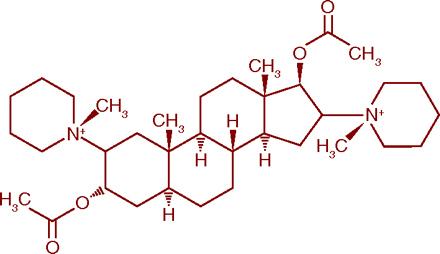
Bovet and colleagues synthesized a series of simpler compounds chemically related to curare, leading to the discovery in 1947 of gallamine, a short-acting competitive neuromuscular blocker (14). Several other competitive agents were developed culminating with pancuronium, which was synthesized by Hewett and Savage in 1964. Five times more potent than curare, pancuronium was introduced commercially in 1968 and became the drug of choice, both therapeutically and as a component of the three-drug cocktail used in lethal injection executions. The persistent blockade and difficulty in reversing relaxation after surgery associated with curare and pancuronium subsequently led to development of a series of short and intermediate acting competitive blockers (15).
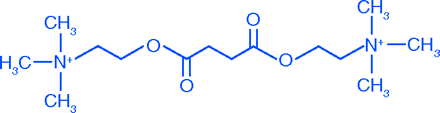
Meanwhile, succinylcholine was re-examined. Hunt and Traveau had studied the effects of various choline esters on blood pressure in 1906, but their animals were “curarized” and they failed to observe succinylcholine’s muscle relaxant effects (16). Four decades later, workers in Great Britain, Italy, and the United States independently described the neuromuscular blocking activity of succinylcholine (17). Because of its rapid onset and hydrolysis, succinylcholine, a depolarizing blocker, is still used as a short-acting, controllable muscle relaxant.
Prescott and Smith after Their Curare Experiences
After publishing their reports on curare, Prescott and Smith both moved on to other interests and led long, productive professional careers. Working at Burroughs Wellcome for more than twenty years, Prescott was responsible for launching a number of the company’s products in the UK, including methedrine, pethidine, and amidone, as well as d-tubocurarine. During this time, he also served on the Action and Uses Committee of the British Pharmacopoeia. He was a member of the Royal College of Physicians and the British Pharmacological Society and was elected a Fellow of the Royal Society of Chemistry and the Royal Society of Medicine. With Franklin Bignell, Prescott coauthored the pioneering treatise, Vitamins in Medicine, which was published in several editions and, though now out of print, is still cited as a seminal compendium of vitamins. He died in 1989.
Smith continued as head of the University of Utah’s anesthesiology department until 1954, when the medical school dean moved to install a full-time faculty. Preferring to continue his clinical practice, Smith relinquished his leadership of the department but remained an associate clinical professor of anesthesiology. In 1956, he served as president of the American Society of Anesthesiologists, and in 1986 he received the Distinguished Service Award of the Utah Society of Anesthesiologists (18). He maintained an active private practice at LDS Hospital until his retirement in 1980 and died in 1987 (19).
Although Richard Gill continued to advocate expanded therapeutic uses for curare until his death in 1958, anesthesiologists rapidly moved on to newer muscle relaxants. Tourists now regularly visit the secondary rain forests where small towns, winding roads, and a few airports occupy areas that had been remote and formidable to Gill. But, deep in the primary rain forests of the Amazon basin, vanishing breeds of indigenous tribes still coexist with the jungle. They still make curare paste from tropical vines and still use it to kill game with their blow darts (8).
Acknowledgements
The author wishes to thank Prof. Laurie Prescott for providing documents from his family archives and many helpful details concerning his father. This article also benefitted from documents housed in various archives and generously provided by Dr. Christopher Hilton (Senior Archivist, Wellcome Library), Rachael Johnson (Picture Researcher, Wellcome Trust), Roy Webb and Clint Bailey (Special Collections, J. Willard Marriott Library, University of Utah), David Allen (Library Collections Coordinator, Royal Society of Chemistry), Karen Schlaegel (British Pharmacological Society), Erin McGarrigle (Publications Manager, Australian Society of Anaesthestists), and Florence Cepeda and Dr. Selma Calmes (Arthur Guedel Memorial Anesthesia Center, Health Sciences Library, California Pacific Medical Center)
- Copyright © 2010
References

Rebecca J. Anderson, PhD, holds a BA in chemistry from Coe College and her doctorate in pharmacology from Georgetown University. After several industry positions in pharmaceutical research and development, she now works as a technical writer and is the author of Career Opportunities in Clinical Drug Research. E-mail rebeccanderson{at}msn.com